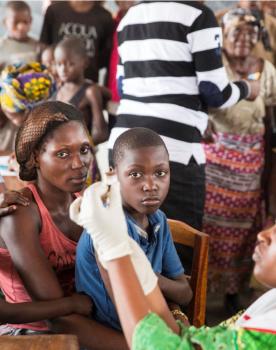
Our projects
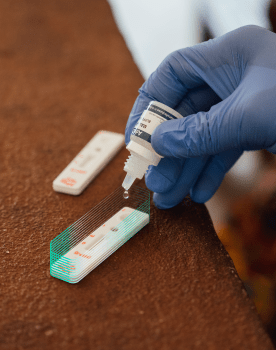
Under-diagnosis and delays in diagnosis or screening are a major public health problem in resource-limited countries.
This is the case, for example, in the management of epidemics, where a late alert and response can considerably increase the number of victims. Delayed diagnosis, meanwhile, reduces the chances of survival, as in the case of cervical cancer.
In concrete terms, these problems can be explained by the following causes:
- Either the product exists but is not available, or is too expensive and/or not adapted to MSF's areas of intervention => The MSF Foundation will work to make it available and adapted to the regions of deployment (equity).
- Or the tool does not exist, and we need to create this new medical diagnostic device. (discovery)
The projects in this field create tools and/or implement new practices to meet these challenges.
In low- and middle-income countries, over 50% of patients needing rehabilitation have no access to it. This lack of rehabilitation care can have serious physical, functional, psychological and social consequences for patients. The MSF Foundation and MSF have come to the common conclusion that the supply of rehabilitation care is too limited and non-specialized.
News of our projects