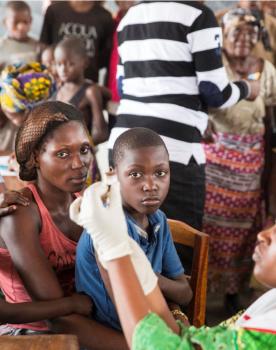3D Program
In brief
The 3D program highlights the use of digital technologies, such as surface scanning, 3D printing, and telerehabilitation—as key tools to improve access to assistive devices for patients in need.
We focus particularly on upper-limb amputees, like in Jordan, where prosthetic arms are fully 3D-printed. We also support burn victims with facial and neck injuries in Jordan, Gaza, Syria, and Haiti, where transparent compression orthoses are produced using the same technologies. Our goal is to provide patients with high-quality devices, along with tailored rehabilitation care.
Since the program began, nearly 500 patients have benefited from these various devices.
Status of the project
News
In detail
Upper Limb Prosthetics
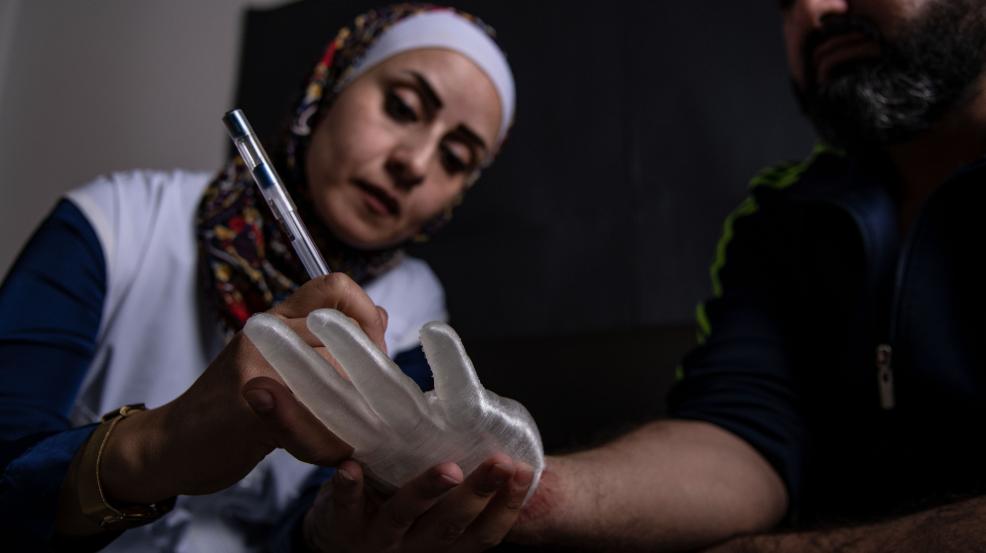
In Amman, Jordan, upper limb prosthetics are now fully 3D-printed. Patients are supported by a multidisciplinary rehabilitation team (physiotherapist, occupational therapist, engineer, and orthotist/prosthetist). In addition to prosthetics, assistive devices or small tools tailored to each patient's specific needs are designed and created to help them in their daily life.
This pilot project in Amman has demonstrated since June 2017 that 3D printing of prosthetics is a deployable, accessible, and adaptable tool for our fieldwork, offering an affordable alternative to conventional manufacturing methods.
Compression Masks
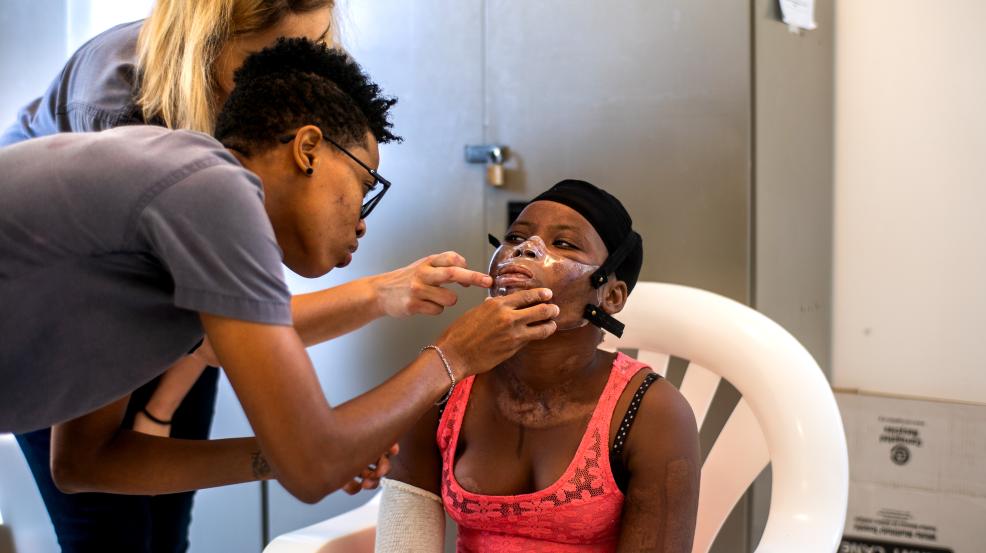
Building on this success, the 3D program expanded to include the design of compression masks for the face and neck of burn victims. It was introduced in Amman in 2018, followed by deployment in Haiti in 2019, Gaza in 2020 (suspended since October 2023), and Syria in 2025.
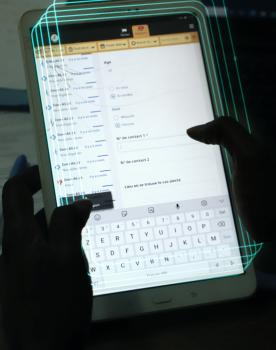
Facial burns can lead to severe long-term consequences (skin contractures and hypertrophy causing functional, aesthetic, and social impacts) if not treated with compression masks and thorough patient follow-up. Here too, 3D technology, particularly surface scanning, enables earlier and more comfortable care compared to conventional methods. This is followed by precise computer modeling, with remote technical support via telemedicine if necessary.
Deployment
The 3D program aims to foster the gradual autonomy of our teams in the field. Initially, they receive training and support from MSF teams, as well as external experts and partners, for designing assistive devices and developing care strategies. Over time, local teams become self-sufficient in using 3D technologies, while continuing to benefit from the Foundation's support. This system also encourages collaboration between the programs in Amman, Haiti, Gaza, and Syria.
In parallel, the Foundation launched a regional 3D project in the Middle East in 2023 to prevent gaps in patient follow-up and develop local care solutions in different regions.
Research Study on Compression Masks in Haiti
Patient follow-up
How does it work?
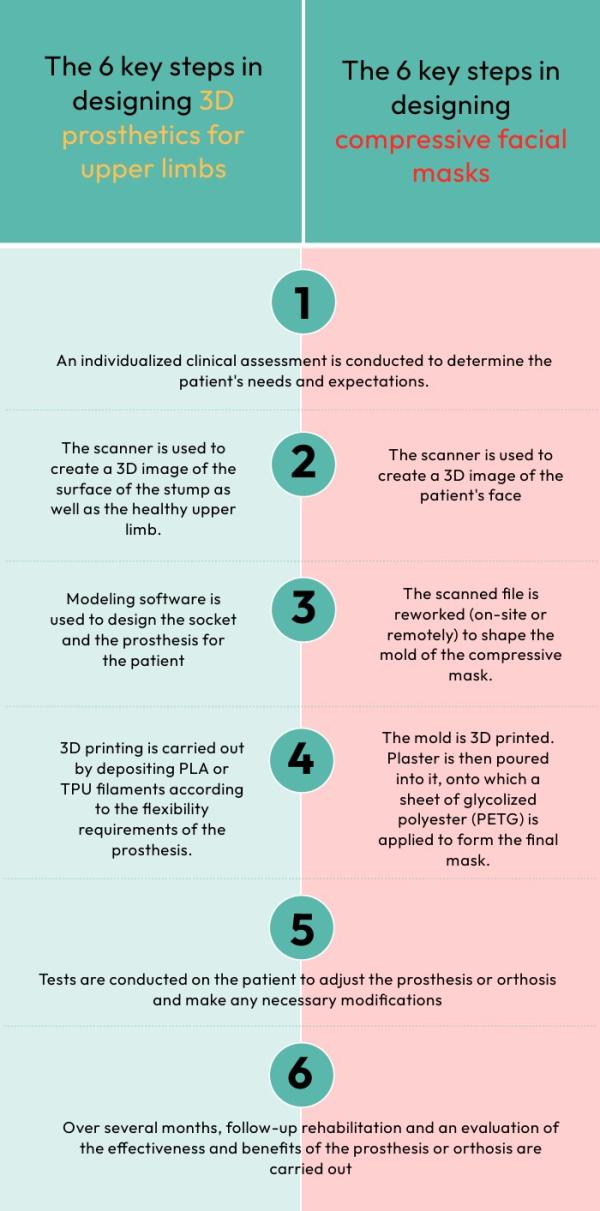
The main stages of the program
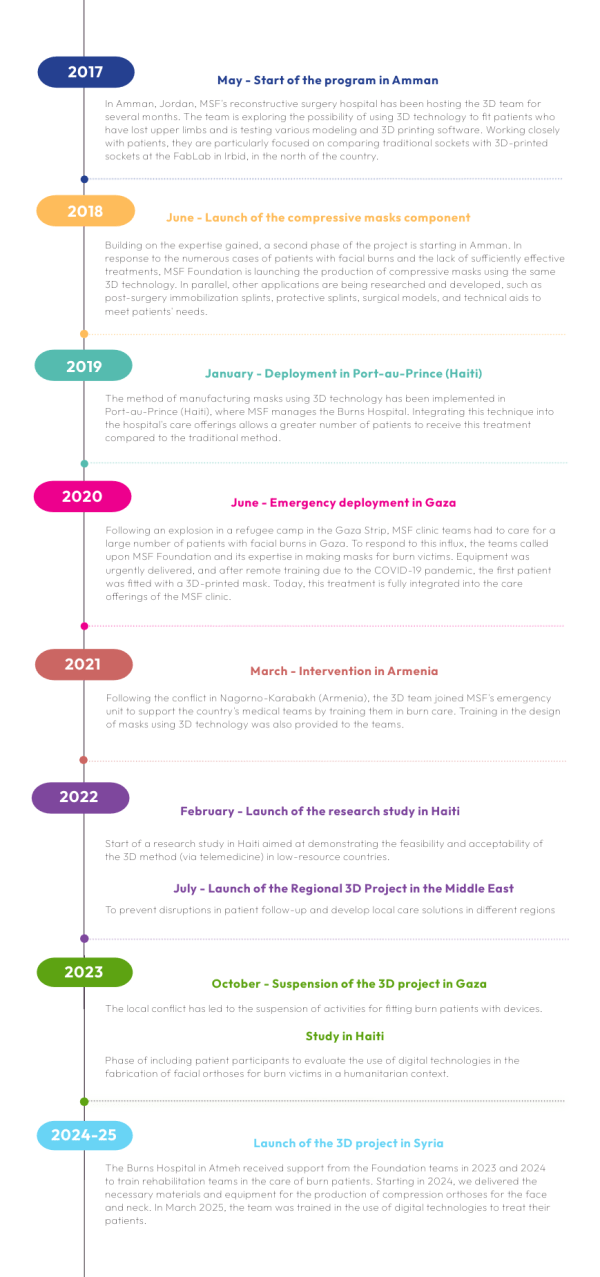
3D programm in pictures
Our partners

Contribute
You wish to specifically support the development of this project ? Contact Catherine Béchereau - Loyalty and Philanthropy Manager 01 40 21 56 88 - [email protected]